Diagnosing patellar syndrome seems easy, but actually, it proves to be relatively complicated. Even if this condition hides behind the majority of knee pain complaints, its diagnosis should remain objective.
Indeed, the patellar syndrome, also called patellofemoral syndrome, is one of the most common knee conditions. It mainly manifests with pain in the joint, between the kneecap and the femur.
EPITACT® reviews the diagnosis of patellar syndrome: who to consult? How and when is the diagnosis established? What solutions once the diagnosis is confirmed?
Diagnosing patellar syndrome: who to consult?
To diagnose patellar syndrome, do not hesitate to act as soon as the first knee pain appears. Consult a health professional who will identify the cause of your pain. He/She can be a general practitioner, a sports physician or an orthopaedic surgeon.
How to diagnose patellar syndrome?
Diagnosing patellar syndrome includes several steps, among which the patient questioning, the clinical examination and the radiological assessment, if necessary.
Anamnesis: first step in the diagnosis
The patellar syndrome symptoms are numerous and vary in intensity but the two main ones are pain and joint instability. Because these symptoms are subjectively perceived by the patient, the practitioner begins the diagnosis with some questions to the patient (anamnesis). The pain associated with the patellar syndrome is mainly located in front of the knee, behind the kneecap. It tends to increase in a sitting position or during repeated flexion/extension movements (e.g.: stairs). This questioning represents the first essential step to diagnose patellar syndrome.
Clinical examination to objectify the pain
Then, the diagnosis of patellar syndrome is based on the patient clinical examination. In other words, the health professional observes the patient to identify the causes of this pain. The aim is to assess the normal or abnormal functioning of the knee and the possible presence of associated conditions(5).
The practitioner generally begins with walking assessment. He subsequently analyses the alignment of lower limbs and the morphotype of the patient (for example, genu valgum(1)). To do so, the patient is standing, in underwear, feet parallel. If necessary, he’s asking to take certain positions like squats to find an eventual muscle weakness (particularly quadriceps and abductors)(5).
The practitioner also practices palpation of the patient to identify the precise location of pain. Doing patella tests could also be required to assess knee instability or the presence of patellofemoral osteoarthritis.
Radiological assessment to confirm the hypothesis
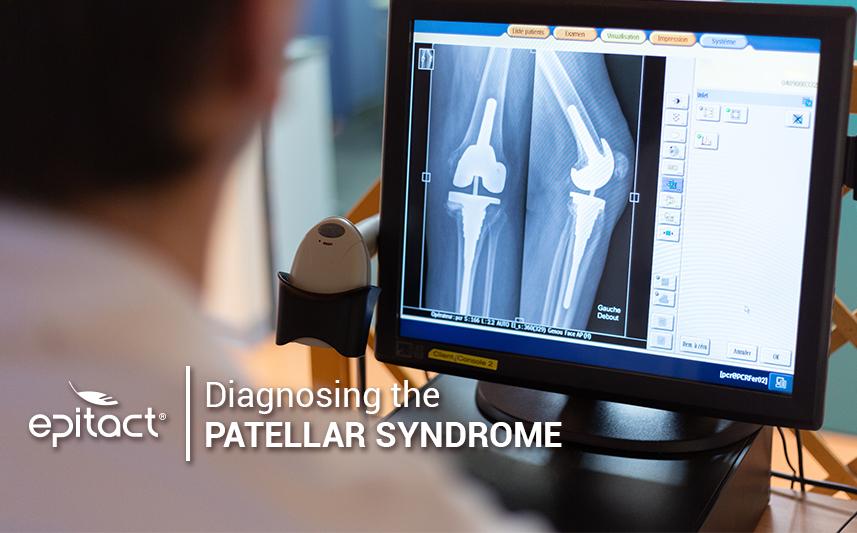
Diagnosing patellar syndrome proves to be difficult because of the number of possible associated conditions. Therefore, the objective consists in excluding these differential diagnoses. Since the symptoms of the patellar syndrome aren’t pathognomonic, imaging allows to eliminate some other hypotheses. Before radiological assessment, the clinical examination aims to reduce the possibilities. For example, a subluxation, a patellofemoral dysplasia or a poor positioning of the kneecap(2) could be excluded.
Next, medical imaging captures knee X-Rays images from front, profile, weight-bearing and then flexed at 30°(1). MRI can also be required to determine the presence of a cartilage or soft tissues lesion for example(3). The last possible associated conditions will be excluded or confirmed: patellar tendinopathy, fracture, Sinding-Larsen-Johansson disease or Osgood-Schlatter disease among others(3, 4).
When to consult in case of knee pain?
Diagnosing patellar syndrome as soon as possible is important due to the insidious nature of the condition. Indeed, chronic pain can rapidly become disabling. In a long-term, it can have moral and psychosocial consequences and affect the patient’s quality of life. Every step in the diagnosis is crucial, the questioning shouldn’t be neglected.
What solutions are proposed?
Preventive solutions
For people subject to patellofemoral pain, preventive solutions exist. EPITACT® has developed knee braces to be daily or occasionally worn during sports activities for example. Find out the PHYSIOstrap™ MEDICAL brace* to secure your knee without impeding movements. Also, discover the PHYSIOstrap™ SPORT brace* that stabilises the kneecap during sports activities.
Curative solutions
Some post-diagnosis solutions are also suggested to relieve pain. Physiotherapy sessions with the physiotherapist aim to strengthen the muscles around the patella. As a complement, resting and wearing insoles can also be recommended. However, surgery is rarely considered.
You’d understand, diagnosing patellar syndrome may seem easy but its pathway is actually much more complex. To better understand this condition, learn how to prevent and treat it, and why it is so frequent among sportspersons.
*These products are class I medical devices that bear the CE marking under this regulation. Carefully read the instructions before use. Manufacturer: Millet Innovation. 09/2021
For more details about this general and simplified approach, here are further sources:
(1)Tamalet, Bertrand, Pierre Rochcongar, et Goulven Rochcongar. « La fémoro-patellaire : une articulation oubliée ? » Revue du Rhumatisme Monographies, Pathologies du genou - Première partie, 83, no 2 (1 avril 2016): 71 77. https://doi.org/10.1016/j.monrhu.2016.01.005.
(2)Goux, P Le. « Démembrement clinique et approche thérapeutique des syndromes rotuliens - Clinical analysis and treatment of the patellofemoral syndromes ». Mise au point, La Lettre du Rhumatologue, no 315 (2005): 5.
(3)Fournier, Dr Yann. « Le Syndrome Douloureux Rotulien ». Centre orthopédique Santy, 2015. http://orthopedie-lyon.fr/wp-content/uploads/2012/02/DIU-SPORT_-LYON_-SYNDROME-DOULOUREUX-ROTULIEN_DR-FOURNIER-min.pdf.
(4)Baptiste Claudon. Phénomène d’adaptation cinétique lors de la marche du patient présentant un syndrome femoro-patellaire douloureux : mise en évidence et réversibilité sous traitement de rééducation. Sciences du Vivant [q-bio]. 2010. hal-01733971
(5)Willy RW, Hoglund LT, Barton CJ, et al. Patellofemoral pain: clinical practice guidelines linked to the International Classification of Functioning, Disability, and Health from the Academy of Orthopaedic Physical Therapy of the American Physical Therapy Association. J Orthop Sports Phys Ther. 2019;49(9):CPG1–CPG95. doi:10.2519/jospt.2019.0302.
 Pharmacie
Pharmacie